Search
Age-specific definitions for acute respiratory distress syndrome (ARDS) are available, including a specific definition for neonates (the "Montreux definition"). The epidemiology of neonatal ARDS is unknown. The objective of this study was to describe the epidemiology, clinical course, treatment, and outcomes of neonatal ARDS.
We aimed to develop and validate a prediction table for a simplified measure of rightward shift of the fetal oxyhaemoglobin saturation (SpO2) versus inspired oxygen pressure (P IO2) curve as an objective marker of lung disease severity in very preterm infants, independent of unit altitude or oxygen prescribing policies.
Right shift of the peripheral oxyhaemoglobin saturation (SpO2) versus inspired oxygen pressure (PIO2) curve is a sensitive marker of pulmonary gas exchange. The aim of this study was to assess the impact of prematurity and bronchopulmonary dysplasia (BPD) on gas exchange and right-to-left shunt in the neonatal period, and its evolution over the first year of life.
Evidence suggests that intramuscular vitamin A reduces the risk of bronchopulmonary dysplasia (BPD) in preterm infants. Our objective was to compare enteral water-soluble vitamin A with placebo supplementation to reduce the severity of BPD in extremely preterm infants.
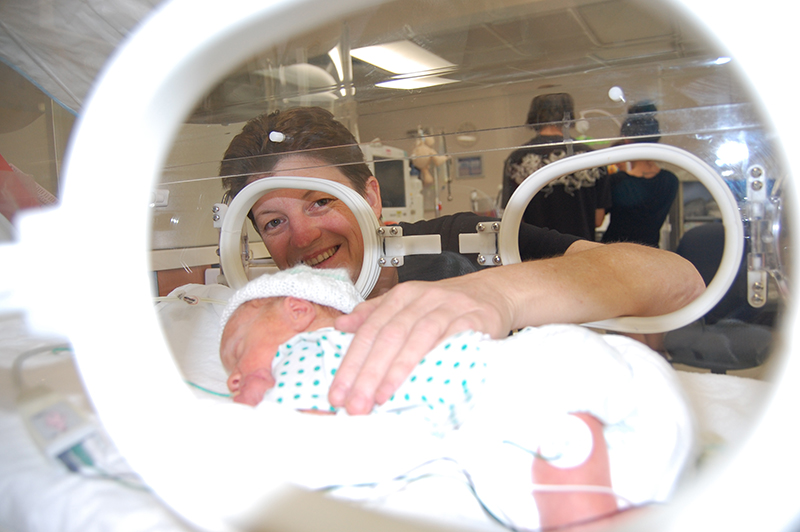
The Chronobiology team works to understand the factors that contribute to poor lung and heart function in newborn infants and find ways to prevent heart and lung disease.

Head, Developmental Chronobiology

Meet the team behind the CIRCA DIEM study.
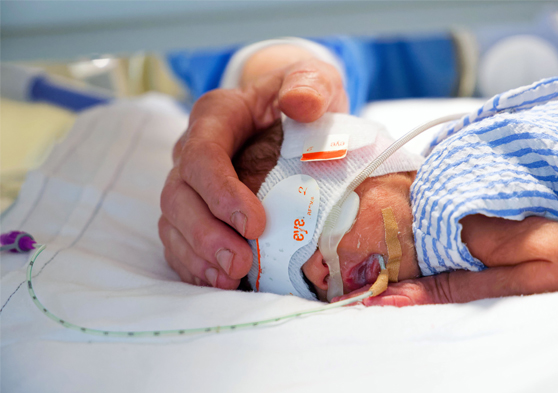
A sub-study is an ‘add-on’ study that helps to answer specific questions within a larger research project. If you decide to participate in the CIRCA DIEM study, you or your child may be invited to take part in one of the CIRCA DIEM sub-studies.

The CIRCA DIEM study aims to establish if cycling environmental light and noise levels for premature infants during their initial hospital stay leads to earlier development of circadian (daily) rhythms and better outcomes for the preterm babies, including improved brain development.
